
Covid-19 pandemic: We must plan using models, act on actual data
8 June 2020
COVID-19
Models need to be adjusted by actual measurements, like the actual number of people who are dying from the disease. This means that models tend to be more inaccurate in the beginning, but get better at making predictions over time.
When dealing with Covid-19, South Africa needs to be guided by models in planning for the future, but should rely on actual data in acting now. Models give us a “best guess estimate” of the future, while actual data, although it has limitations, is based on what we actually know.
The South African government relies on models from well-established modellers that suggest we will have at least 40,000 deaths and about 1.2 million symptomatic cases by September 2020. On the other hand, a group of non-affiliated modellers, called PANDA, assert confidently that South Africa will not experience this level of Covid-19-related deaths, and that it is unlikely we will exceed 10,000 deaths as a result of this pandemic. Whom then to believe?
In many ways, this confusion is understandable. This is a new epidemic, and we are still learning about how it spreads in different communities. It is worth remembering the early days of the HIV epidemic. Initially, models assumed that every country would experience the same types of epidemics. This led to estimates of over five million people infected in India, when we now know that the real number is fewer than half of that.
All models use assumptions, which are refined over time. These include the likelihood of viral transmission between people and the percentage of the population who are susceptible to infection. Since most models assume the latter number to be 100%, the models tend to suggest very high numbers of cases and deaths.
Models need to be adjusted by actual measurements, like the actual number of people who are dying from the disease. This means that models tend to be more inaccurate in the beginning, but get better at making predictions over time. This is no reflection on the skill or intention of the modellers, but a natural process of how our understanding increases as epidemics progress.
Governments have to use models to guide their planning, but need to accept that these models will almost certainly be incorrect. As the PANDA actuaries have noted, our population is much younger than those of Europe and North America, and this may affect the course of the epidemic.
We also don’t know the factors that facilitate the spread of this virus. Regions and countries have experienced quite different types of epidemics, for reasons we don’t fully understand. On the other hand, it would be foolish to ignore what has happened in Italy, Spain, the UK and indeed Cape Town. When this virus spreads exponentially, the consequences are dramatic.
So, what real data can we use to track the course of the epidemic? There are three critical measures for us to use:
- The rate of new cases (a measure of spread)
- The stress on the health system
- The amount of testing we are doing, and the percentage of positive tests
What all countries are trying to avoid is uncontrolled and explosive community transmission of Covid-19. That is why we had lockdowns, why we use physical distancing, wear masks etc. Can we determine when extensive community transmission is happening? If you look at the graph of new cases over time, you can see that it is only the Western Cape with new infection rates consistently above 10 per 100,000 of the population. Anything above five by this measure indicates a severe epidemic.
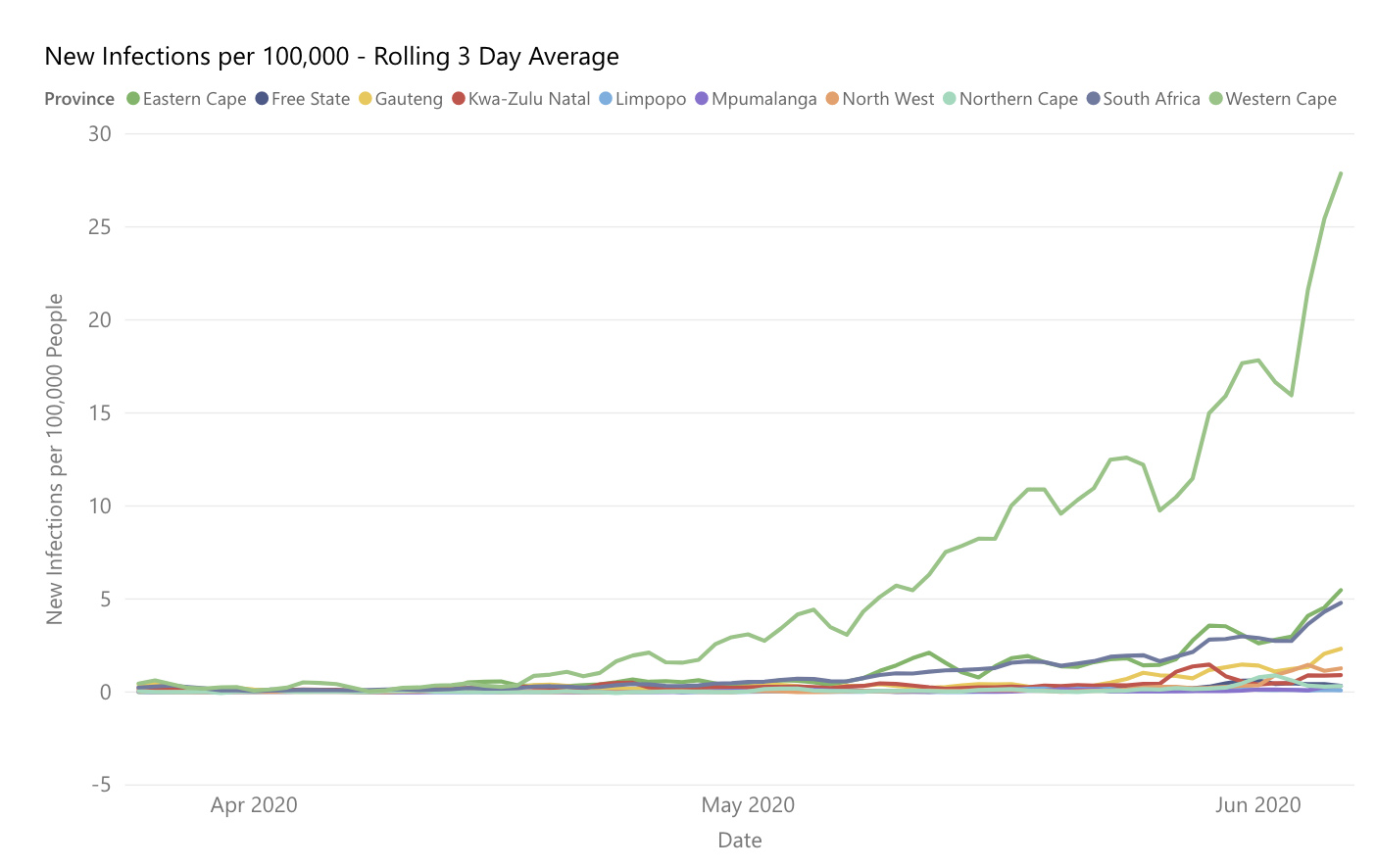

Source: https://www.genesis-analytics.com/covid19/flattening-the-curve
It is worthwhile asking why the Western Cape, and Cape Town in particular, is having such a severe epidemic? It seems unlikely that this is due to more testing, since other provinces, like Gauteng, are also testing at a high rate, and we are seeing the Cape Town ICUs filling up rapidly.
It is more likely a combination of being at an earlier stage, due to exposure to tourism, and a few large cluster events that spilled over into the community. However, given that Cape Town is also the epicentre of South Africa’s TB epidemic, there may be socio-economic factors at play that make this population particularly susceptible to respiratory infections.
It is worth remembering that the measurement of new cases does depend on how much testing we are doing, how quickly those tests are reported and the accuracy of the tests. This is why it is better to view the trend over a few weeks and avoid making decisions based on one or two days of results.
Countries that have experienced severe epidemics have found their health systems flooded and overwhelmed, especially their high-care and ICU units. However, we also need these units for routine post-surgical care. It is therefore helpful to know how close we are to reaching peak ICU capacity.
Genesis has created a simple calculator to try to measure this, which allows a user to enter the number of cases and ICU beds in an area, and then calculates whether the system is about the reach capacity (try it out here). Using this tool suggests that the Western Cape will soon reach peak ICU capacity, with over 1,000 patients requiring intensive care of some sort over the next two weeks.
On the other hand, Gauteng is likely to have fewer than 200 patients who require intensive care over the next two weeks, far below our ICU bed capacity. The Eastern Cape, shown below, has a limited number of ICU beds, and given the state of its epidemic, it can expect to start seeing ICU beds being increasingly limited over the next two weeks.

The last measure to consider is testing. At the moment, South Africa is doing about 20,000 tests a day, and by far the most tests of any African country. The WHO has declared that countries need to have positive tests below 5%, in order to consider their epidemics contained. South Africa’s positivity rate currently stands at 7.5%, but that is being driven by the Western Cape at 17.5% and the Eastern Cape at 9%. The other provinces have positivity rates of less than 2%.
It is still unclear how the Covid-19 epidemic will progress in South Africa, despite all the modellers’ predictions. Part of this uncertainty is the unknown of the virus, but the other part is the fact that our action, or inaction, will impact its spread.
We need to keep maintaining our surveillance of this epidemic and respond to the data in some of the following ways:
- In areas like Cape Town, with extensive community transmission, we may have missed the boat for a test-and-trace approach. Authorities need to focus on working with communities to ensure that sick people isolate themselves, that their contacts quarantine for two weeks, and that sufficient ICU capacity is in place to treat people with acute respiratory distress. There must be rigid adherence to the use of masks and physical distancing. What is presently happening in the Eastern Cape is extremely worrying, and the national Department of Health should consider intervening
- In areas with an increase of new cases, we should be aggressively tracing all the contacts of cases, and ensuring that they are tested and quarantined
- Areas that do not show an increase in new cases should be allowed to operate within the existing regulations of safe commuting, safe workspaces, etc. Schools should be allowed back and businesses allowed to operate fully. But the situation needs careful monitoring
- All health workers should have access to PPE. The Department of Health should use this opportunity to enter into a constructive partnership with the private sector. Goodwill needs to be demonstrated on both sides, otherwise this does not bode well for the National Health Insurance in the future
And of course, to all of us: Keep physically distancing, wear your masks, keep washing your hands and stay home if you are sick. DM/MC
Saul Johnson is managing partner of the Health practice at Genesis Analytics